What to do about Antibiotic Resistant Bacteria?
Yikes, Superbugs!
Antibiotic-resistant strains of Superbugs (bacteria) are evolving as we speak--for several reasons. First, huge quantities of antibiotics are routinely given to livestock that we use as food. In the short term, this practice increases profit margins for Agribusiness. Any factory farm manager who chooses to be prudent in his antibiotic usage will find himself at a disadvantage, because his animals will grow a bit slower than those of his competitors.
But we're also shooting Public Health in the foot.
On balance, the practice of megadosing our livestock with antibiotics is uneconomic--even if it is consistent with Free Market Economics.
A second problem is patient compliance. Many years ago, I had some dental work done. I was given a prescription for an antibiotic, together with instructions about how much to take, and when to take it.
I took it for a few days, and after no infections developed, I threw out the meds. Like most people, I was not aware of the problem of antibiotic-resistant bacteria. If a few of the beasties had survived, I would have had a new problem. The surviving bacteria would have developed some resistance to the antibiotic that I had been taking. And I would have needed to switch to a different, more expensive antibiotic.
If I had passed on the Superbug to another person without his being aware of the source, the standard antibiotic treatment would have been less effective--perhaps even ineffective. Then his physician would need to switch to a Plan B antibiotic. The upshot: His infection would last longer than it would if I had simply followed the written directions on my antibiotic prescription.
Third, some patients with viral infections pester their physicians for antibiotics--even though these medications have no known antiviral effects. And many doctors cave in to the unreasonable requests.
A fourth Superbug problem is related to HIV/AIDS. Like immunosuppressive drugs that prevent the rejection of transplanted organs, HIV can compromise the immune system to the extent that HIV patients are much more vulnerable to infections of all kinds. Standard courses of antibiotics will not necessarily knock out the opportunistic infections. As a result, HIV patients are more likely to spread infectious, antibiotic-resistant bacteria than people with normal immune systems.
Even with judicious use of antibiotics, most harmful bacteria will eventually adapt. The inevitable result is Superbugs.
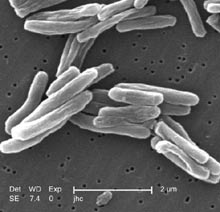
One of the Superbugs in the pipeline is multi-drug-resistant Tuberculosis. In the Bad Old Days, before antibiotics, TB killed an awful lot of people. It's still a problem in developing countries, where ordinary people do not have sufficient access to baseline health care. And TB is poised to make a comeback in the developed countries. That's one of several reasons why unrestricted immigration to the developed countries is not practical.
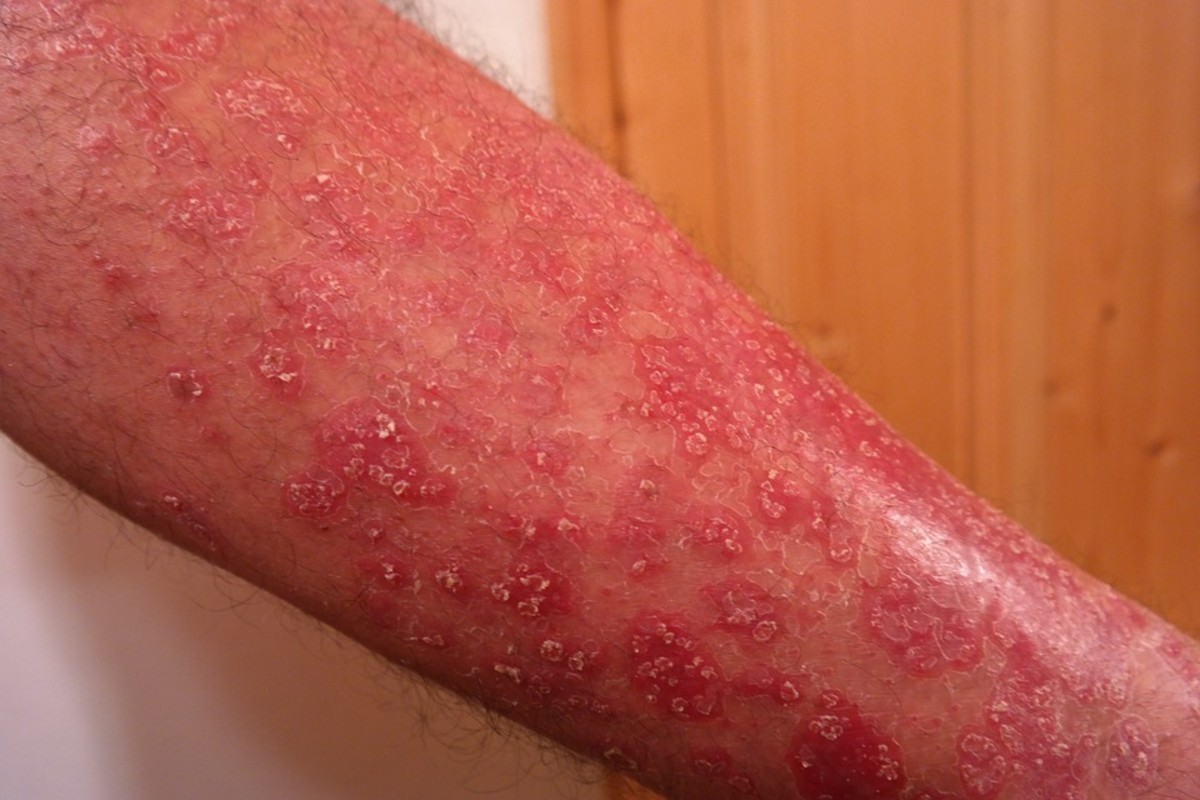
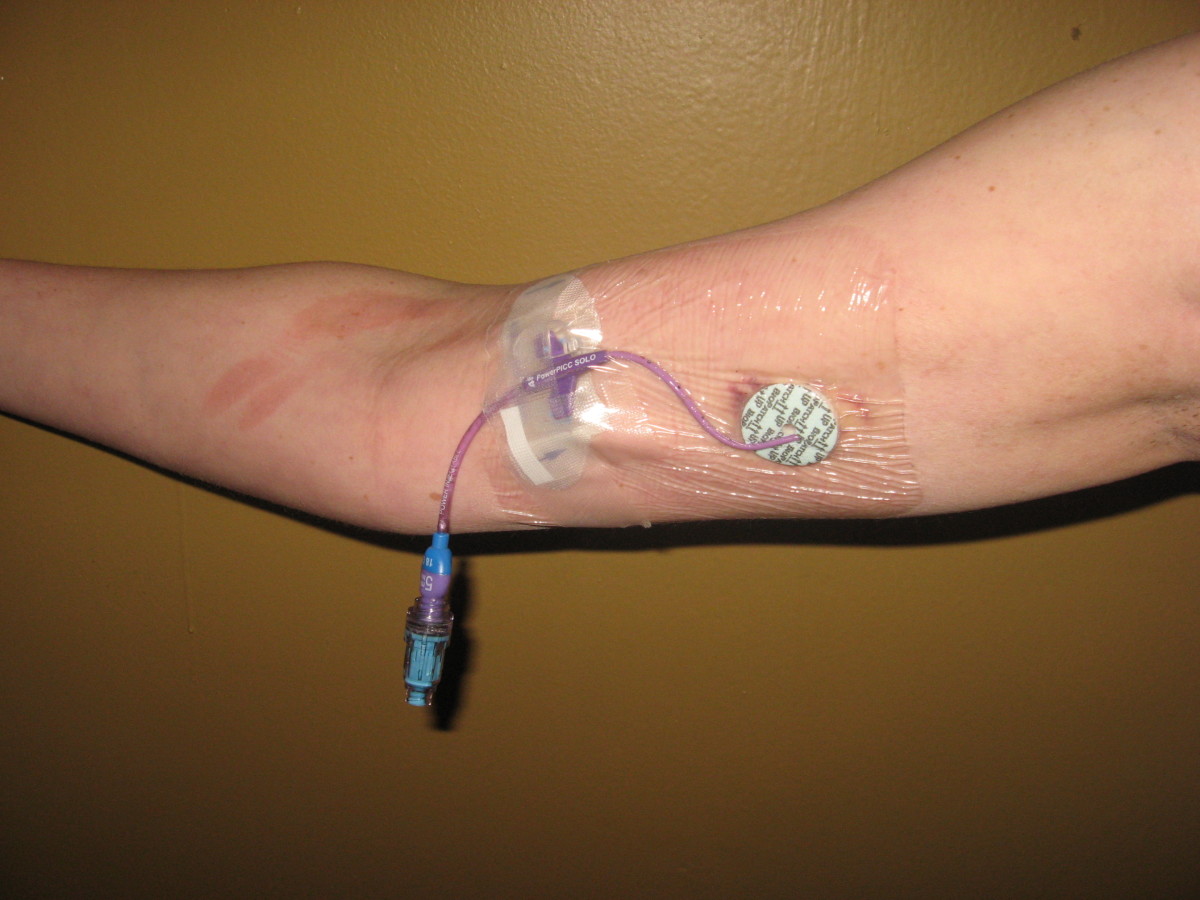
Another Superbug concern is MRSA (Methicillin-resistant Staphylococcus aureus). This is a big problem in hospitals, nursing homes, and other institutional settings.
Invasive non-typhoidal salmonella (iNTS) is antibiotic resistant. And some strains of Gonorrhea are resistant to penicillin. Here's a recent headline:
Scientists find new superbug spreading from India
Houston, we have a problem.


Research and rotation
There are a few things that governments of the developed countries can do about Superbugs. First, we need more government regulation of antibiotics given to livestock. Western European governments--especially Denmark--are more serious about managing the problem of antibiotic overuse in farm animals than we are. Of course, they don't have 100% compliance.
Nevertheless, it's better than the American laissez-faire approach. It's unfortunate that the same European governments are so inept at managing their economic problems. Oh well, being part smart is better than being totally brain-dead.
Second, governments should subsidize research on new antibiotics, on a Cost Plus basis.This was one of the proactive cost-containing measures that the American government took during World War II. Defense contractors were allowed to make a reasonable profit, but there weren't a whole lot of $400 hammers--I mean 'hand-held impact devices'--at that time. In the spirit of Cost Plus, there should be no new antibiotic patents or other corporate welfare for pharmaceutical companies who research new antibiotics on the government's dime.
Why have such a subsidy in the first place? Because the necessary level of research on new antibiotics is simply not being done. Presumably, because the projected profits are too small.
When the inevitable diminishing returns hit older antibiotics, they should be completely withdrawn from the world market for many years. Eventually, the older antibiotics could be reintroduced. But I'm not sure how long the waiting period would be. 10 years? 30 years? 100 years? What's my rationale for reintroduction?
Resistance to Antibiotic X--in the absence of environmental Antibiotic X--is excess genetic baggage for bacteria. In the long term, Antibiotic X-resistant bacteria living in an Antibiotic X-free world will have a small genetic survival handicap. The bacteria that are NOT trundling around with antibiotic 'armor' will be slightly leaner and meaner.
Given sufficient time, the latter bacteria will out-reproduce the strains with resistance to Antibiotic X, until the populations of the former strain are essentially extinct. This isn't rocket science. We're talking Evolutionary Biology 101 here. At this point, Antibiotic X will have regained 99% of its full former potency--temporarily.
Thus, it's not necessary to mothball old antibiotics indefinitely. Continued research, coupled with a rational rotation routine, is a vital long-term strategy.
Copyright 2013 by Larry Fields